Ingrown Toenails
Ingrown Toenails Treatment in Las Vegas, NV
Our podiatrists treat ingrown toenails in the area of Las Vegas, NV. Call our office today at (702) 213-9093 if you are dealing with ingrown toenail.
An ingrown toenail is a toenail that grows sideways into the nail bed, causing pain and swelling. Ingrown toenails can worsen and cause drainage, turning into a serious infection.
Symptoms of Ingrown Toenail
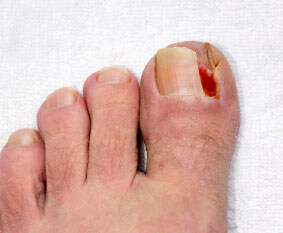
Signs that may indicate the formation of an ingrown toenail include redness, pain, swelling of the surrounding skin, possible bleeding or oozing of pus, and an overgrowth of the skin around the nail. The surrounding skin may also feel tender and become swollen or hardened. Most ingrown toenails are diagnosed by a simple physical exam; however, an x-ray may be required to show how deep the nail has grown into the skin of the toe.
Causes of Ingrown Toenails
Many factors influence the likelihood of developing an ingrown toenail. The most common way ingrown toenails are formed is due to an incorrect method in how the toenails are trimmed. If you cut your toenails too short or cut them at an angle, you’re putting yourself at risk of getting this condition. Another main factor that contributes to ingrown toenails is the choice of footwear. Those who commonly wear tightly fitted shoes, such as high heels, that do not give the toes enough room, put too much pressure on the big toes. This can create an ingrown toenail. To alleviate the pain, a small piece of cotton may be fitted underneath the nail. However, in more serious cases, total removal of the nail may be necessary.
How to prevent ingrown nails
Ingrown toenails can be preventable with certain measures. For starters, allowing your toe nails to grow slightly longer in length will help prevent them from becoming ingrown. If you have already developed an ingrown toenail, soak the affected toe in warm water. This will alleviate the pain and help prevent an infection from forming. Antibiotic soap or Epsom salts may be added to further help the relieving process and avoid infection. Placing cotton beneath the affected area is also suggested, as this may help the toenail grow upwards and not into the nail bed. Swelling and redness can be reduced by resting with your feet elevated.
A podiatrist should be seen if the pain becomes so serious that it prevents you from doing your everyday activities. If a red streak running up your leg appears or if you suspect your infection has spread, contact a podiatrist immediately. Fast treatments can be undertaken to lessen your pain and have you walking comfortably.
Ingrown Toenails Treatment
Treatment for an ingrown toenail varies between patients and the severity of the condition. In most cases, it is best to see your podiatrist for thorough and proper treatment. After examining your toe, your podiatrist may prescribe oral antibiotics to clear the infection if one is present. In more serious cases surgical removal of either a portion of the nail or the entire nail may also be considered. In some cases, complete removal or destruction of the nail root may be required. To prevent the nail from growing back, medication will be placed directly into the nail bed. This procedure would be performed under local anesthesia and is a faster method to alleviate discomfort from an ingrown toenail. Most patients who undergo nail surgery experience minimal pain afterward and can return to normal activity the following day. For a proper diagnosis and advised treatment plan, we recommend you seek the care of a podiatrist as soon as you notice the warning signs of an ingrown toenail.
Hammertoes & Crooked Toes
A hammertoe is commonly mistaken as any type of toe deformity. The terms claw toe, or mallet toe, although technically different than a hammer toe, are commonly referred as such. The toe may be flexible with movement at the joints, or it may be rigid, especially if it has been present for a long time. With a true hammertoe, the deformity exists at the proximal interphalangeal joint only. The true mallet toe has its deformity at the distal interphalangeal joint only and more commonly causes a callous on the tip of the toe as pressure is placed there. The true claw toe is a combination of the hammer and mallet toe deformities and involves both joints of the toe. If the big toe (hallux) has a hammertoe, it is more commonly called a Hallux Hammertoe and may be treated somewhat differently than described here. Symptoms of a hammertoe are usually first noticed as a corn on the top of the toe or at the tip which produces pain with walking or wearing tight shoes. Most people feel a corn is due to a skin problem on their toes, which in fact, it is protecting the underlying bone deformity. A corn on the toe is sometimes referred to as a heloma dura or heloma durum, meaning hard corn. This is most common at the level of the affected joint due to continuous friction of the deformity against your shoes. A soft corn, or heloma molle, may also exist in the web space between toes. This is more commonly caused by an exostosis, which is basically an extra growth of bone possibly due to your foot structure. As this outgrowth of excessive bone rubs against other toes, there is friction between the toes and a corn forms for your protection.
Causes of hammertoes are usually structural in nature. Many times this is the foot structure you were born with and other factors have now made it so that symptoms appear. The muscles in your foot may become unbalanced over time, allowing for a deformity of the small bones in each toe. With longstanding deformity, the toe may become rigid. Sometimes one toe is longer than another and this causes a buckling of the digit. A hammertoe may also be caused by other foot deformities such as a bunion. Trauma or other surgery of your foot may predispose you to having the condition if your foot structure is altered. Prevention of a hammertoe can be difficult as symptoms do not arise until the problem exists. Wearing shoes that have extra room in the toes may eliminate the problem or slow down the deformity from getting worse. Sometimes surgery is recommended for the condition. If the area is irritated with redness, swelling, and pain some ice and anti-inflammatory medications may be helpful. The best prevention may be to get advice from your podiatrist. Podiatric care may include using anti-inflammatory oral medications or an injection of medication and a local anesthetic to reduce this swelling. When you go to your doctor, x-rays are usually required to evaluate the structure of your foot, check for fractures and determine the cause. The podiatrist may see you to take care of any corns that develop due to the bone deformities. They may advise you on different shoewear or prescribe a custom made orthotic to try and control the foot structure. Padding techniques may be used to straighten the toe if the deformity is flexible, or pads may be used to lessen the pressure on the area of the corn or ulcer. Your podiatric physician may also recommend a surgical procedure to actually fix the structural problem of your foot.
urgery to correct for a hammertoe may be performed as an outpatient procedure at a hospital, surgery center, or in the office of your podiatrist. There are multiple procedures that can be used depending on your individual foot structure and whether the deformity is flexible or rigid. There may be a surgical cut in the bone to get rid of an exostosis, or a joint may be completely removed to allow the toe to lay straight. Sometimes when the joints are removed the two bones become one as they are fused in a straightened position. Many times one toe will be longer than another and a piece of bone is removed to bring the toes in a more normal length in relation to each other. Sometimes tendons will be lengthened, or soft tissue around the joints will be cut or rebalanced to fix the deformity. Angular corrections may also be needed. The surgeon may place fixation in your foot as it heals which may include a pin or wires. MIS Surgery for fixing of hammertoes.
Hallux Limitus & Rigidus
This is arthritis of the big toe joint (metatarsal phalangeal joint) which is graded by it’s severity: Stage 1 – Mild arthritis with inflammation, swelling and some pain which is usually not constant. Stage 2 – Moderate arthritis with a limitation in the range of motion of the big toe joint and aggravated with activity and high heels. X-rays will show spurring and some loss of joint space. Sesamoids can be affected. Stage 3 – Severe arthritis with almost complete loss of joint space on x-ray and constant pain. Sesamoids are almost always involved. Stage 4 – No joint space.
Treatment Options:
Stage 1 – NSAIDS, Rx Topical Medication, Laser, ICE and Orthotics management. Stage 2 – Same as Stage 1 but if fails may consider injection of Amniotic fluid (insurance usually won’t cover this) Surgery in the form of a cheilectomy, which is a removal of the arthritis/spurs by removing it with surgical equipment. Not always definitive. Also may consider an osteotomy of the metatarsal or phalanx depending upon the structure of the foot. Stage 3 – Can try amniotic fluid injection but this will not cure it, may last for 6 months to a year. Can inject over and over if you like this treatment. Surgical-osteotomy of bone to shorten or lower with or without implant. Implant into one side of the joint or both. This is surgeon preference based on patient activity level and x-rays. Fusion is an option as well but this will cause permanent loss of motion to the joint but will relieve all pain in 95% of patients. Stage 4 – Fusion or Implant.
Post Operative Courses for Above Surgical Options:
Cheilectomy – 48 hours stay off foot and elevate and ice. PT. Dynasplint (medical device to wear at home covered by insurance) Then wear boot for 2-3 weeks, then back in sneakers till 6 weeks or so then regular shoes to tolerance. We recommend post op cold laser treatment to speed recovery. Topical pain meds. Osteotomy With or Without Implant – Stay off for 48 hours completely, elevate and ice. Wear cam walker boot for 4-6 weeks. PT and Dynasplint. Topical pain medication, cold laser therapy. Back in regular shoes around 8-10 weeks. Return to full activity around 3-4 months depending on activity level. Can swim or do stationary bike after 4-6 weeks. Implant – 48 hours ice and elevate, start walking in cam walker boot for 1-2 weeks then wear sneaker at 3-4 weeks will depend on swelling. Return to full activity in 6-8 weeks. Laser, topical cream and PT and Dynasplint post op.
Foot & Ankle Arthritis Treatment
When you think of arthritis you don’t always think of the feet or ankles. Most of us are aware of arthritis in the hands and knees. Well, arthritis does not stop at the knees.
What exactly is arthritis? By definition, it is an inflammatory process of a joint. Initially, the joint or joints can become swollen and the surrounding capsule can become inflamed. Over time the joint will start to break down because of the inflammatory process and the cartilage will deteriorate and eventually the joint can be bone on bone which can be very painful. There are really 2 types of arthritis:
1) Osteoarthritis – which is a breakdown of the joint due to injury or just wear and tear. It affects 10% of the population. In the foot or ankle, this is quite common and you see this in the older population or in athletes. Osteoarthritis is most common in joints that bear weight — such as the knees, hips, feet, and spine. It often comes on gradually over months or even years. Except for the pain in the affected joint, you usually do not feel sick, and there is no unusual fatigue or tiredness as there is with some other types of arthritis. Cartilage is a slippery material that covers the ends of bones and serves as the body’s shock absorber. As more damage occurs, the cartilage starts to wear away, or it doesn’t work as well as it once did to cushion the joint. As an example, the extra stress on knees from being overweight can cause damage to knee cartilage. That, in turn, causes the cartilage to wear out faster than normal. This also happens in the ankle and the big toe joints.
2) Rheumatoid arthritis and all other genetic types are the rest – This is more of an immune or inflammatory diagnosis and has many different types with RA being the most common. There are many more that can affect the body. Blood work is often needed to make the diagnosis and sometimes this does not even work. Gout also falls into this category as well and is an inflammatory arthritis that affects the joints due to a problem with protein synthesis in the body. Medication is often needed to treat the symptoms of Gout as there is no cure. Patients with Gout are more difficult to operate on because of the crystals that form in and around the joints.
Patients with severe deformity of their feet due to rheumatoid arthritis can achieve a pain-free foot and be able to wear regular sensible shoes with a forefoot reconstruction procedure. Often times the toes are mangled and the ball of the foot are prominent due to the deformities and breakdown of joints. We can reconstruct the foot and provide full relief of pain and provide you with a much better foot to walk on and wear shoes. Orthotics can also be a great adjunct or a standalone option for some patients.
We are experts in dealing with joint problems of the ankle and the foot. We use state of the art medical and surgical treatment to try and repair or salvage your joints.
In cases where the joints are too far gone, our physicians have been trained on all of the latest implants available in the foot and ankle. Not everyone is a candidate for an implant and careful biomechanical evaluation is needed in order to assess and make sure you are a candidate. The success rate of implants will vary from patient to patient but there is no guarantee that the implants will last forever and sometimes further surgery is needed.
Diabetic Foot Care
Why is it important and even life-saving?
Diabetes is a serious disease that can develop from lack of insulin production in the body or due to the inability of the body’s insulin to perform its normal everyday functions. Insulin is a substance produced by the pancreas gland that helps process the food we eat and turn it into energy. Diabetes affects approximately 23 million Americans and is classified into 2 different types: Type 1 and Type 2. Type 1 is usually associated with juvenile diabetes and is often linked to heredity. Type 2, commonly referred to as adult onset diabetes, is characterized by elevated blood sugars, often in people who are overweight or have not attended to their diet properly. Many complications can be associated with diabetes. Diabetes disrupts the vascular system, affecting many areas of the body such as the eyes, kidneys, legs, and feet. People with diabetes should pay special attention to their feet.
Neuropathy
Of the 23 million Americans with diabetes, 30% will develop foot problems related to the disease. Diabetic foot conditions develop from a combination of causes including poor circulation and neuropathy. Diabetic Neuropathy can cause insensitivity or a loss of ability to feel pain, heat, and cold. Diabetics suffering from neuropathy can develop minor cuts, scrapes, blisters, or pressure sores that they may not be aware of due to the insensitivity. If these minor injuries are left untreated, complications may result and lead to ulceration and possibly even amputation. Neuropathy can also cause deformities such as Bunions, Hammer Toes, and Charcot Feet. It is very important for diabetics to take the necessary precautions to prevent all foot related injuries. Due to the consequences of neuropathy, daily observation of the feet is critical. When a diabetic patient takes the necessary preventative foot care measures, he or she reduces the risks of serious foot conditions. We at The Foot & Ankle Lower Leg Center have the latest treatment options for neuropathy.
Poor Circulation
Diabetes often leads to peripheral vascular disease that inhibits a person’s blood circulation. With this condition, there is a narrowing of the arteries that frequently leads to significantly decreased circulation in the lower part of the legs and the feet. Poor circulation contributes to diabetic foot problems by reducing the amount of oxygen and nutrition supplied to the skin and other tissue, causing injuries to heal poorly. Poor circulation can also lead to swelling and dryness of the foot. Preventing foot complications is more critical for the diabetic patient because poor circulation impairs the healing process and can lead to ulcers, infection, and other serious foot conditions.
Treatment and Prevention
Footwear and orthotics play an important role in diabetic foot care. Orthotics designed with Plastazote foam, the #1 material for protecting the insensitive diabetic foot, are usually recommended. Plastazote is a material designed to accommodate pressure “hot spots” by conforming to heat and pressure. By customizing to the foot, Plastazote provides the comfort and protection needed in diabetic footcare. Footwear constructed with Plastazote is also recommended frequently for the diabetic patient. Diabetic footwear should also provide the following protective benefits:
- High, wide toe box (high and wide space in the toe area).
- Removable insoles for fitting flexibility and the option to insert orthotics if necessary.
- Rocker Soles designed to reduce pressure in the areas of the foot most susceptible to pain, most notably the ball-of-the-foot.
Firm Heel Counters for support and stability. If you are a diabetic, you should be particularly alert to any problems you may be having with your feet. It is very important for diabetics with neuropathy to take necessary precautions to prevent injury and keep their feet healthy. If you have diabetes and are experiencing a foot problem, immediately consult your foot doctor.
Foot Care & Diabetes
Proper foot care is especially critical for diabetics because they are prone to foot problems such as:
- Loss of feeling in their feet.
- Changes in the shape of their feet.
- Foot ulcers or sores that do not heal.
Simple daily foot care can prevent serious problems. According to the National Institute of Health, the following simple everyday steps will help prevent serious complications from diabetes:
- Take Care of Your Diabetes Make healthy lifestyle choices to keep your blood sugar close to normal. Work with your healthcare team to create a diabetes plan that fits your lifestyle characteristics.
- Check Your Feet Every Day You may have foot problems that you may not be aware of. Check your feet for cuts, sores, red spots, swelling, or infected toenails. Checking your feet should become part of your daily routine. If you have trouble bending over to see your feet, use a plastic mirror to help. You can also ask a family member to help you. Important Reminder: Be sure to call your doctor immediately if a cut, sore, blister, or bruise on your foot does not heal after one day.
- Wash Your Feet Every Day Wash your feet in warm, NOT HOT, water. Do not soak your feet because your skin will get dry. Before bathing or showering, test the water to make sure it is not too hot. You should use a thermometer or your elbow. Dry your feet well. Be sure to dry between your toes. Use talcum powder to keep the skin dry between the toes.
- Keep the Skin Soft and Smooth Rub a thin coat of skin lotion or cream on the tops and bottoms of the feet. Do not put lotion between your toes, because this might cause infection.
- Wear Shoes and Socks At All Times Wear shoes and socks at all times. Do not walk barefoot, not even indoors. It is extremely easy to step on something and hurt your feet. Always wear seamless socks, stockings, and nylons with your shoes to help avoid the possibility of blisters and sores developing. Be sure to choose seamless socks that are made of materials that wick moisture away from your feet and absorb shock and shear. Socks made of these materials help keep your feet dry. Always check the insides of your shoes before putting them on. Make sure the lining is smooth and there are no foreign objects in the shoe, such as pebbles. Wear shoes that fit well and protect your feet.
- Protect Your Feet From Hot and Cold Always wear shoes at the beach or on hot pavement. Put sunscreen on the tops of your feet for protection from the sun. Keep your feet away from radiators or open fires. DO NOT use hot water bottle or heating pads on your feet. If your feet are cold, wear seamless socks at night. Lined boots are good to keep your feet warm in the winter. Choose socks carefully. DO NOT wear socks with seams or bumpy areas. Choose padded socks to protect your feet and make walking more comfortable. In cold weather, check your feet often to keep your feet warm avoid frostbite.
- Keep the Blood Flowing to Your Feet Put your feet up when you are sitting. Wiggle your toes for 5 minutes, 2 or 3 times a day. Move your ankles up and down and in and out to improve blood flow in your feet and legs. DO NOT cross your legs for long periods of time. DO NOT wear tight socks, elastic, or rubber bands, or garters around your legs. DO NOT wear restrictive footwear or foot products. Foot products that can cut off circulation to the feet, such as products with elastic, should not be worn by diabetics. DO NOT smoke. Smoking reduces blood flow to your feet. If you have high blood pressure or high cholesterol, work with your healthcare team to lower it.
- Be More Active Ask your doctor to plan an exercise program that is right for you. Walking, dancing, swimming, and bicycling are good forms of exercise that are easy on the feet. Avoid all activities that are hard on the feet, such as running and jumping. Always include a short warm-up or cool-down period. Wear protective walking or athletic shoes that fit well and offer good support.
- Communicate With Your Doctor Ask your doctor to check the sense of feeling and pulses in your feet at least once a year. Ask your doctor to tell you immediately if you have serious foot problems. Ask your doctor for proper foot care tips and for the name of your local podiatrist.
Capsulitis & Metatarsalgia
This is a symptom of a problem with one of the metatarsal-phalangeal joints of the foot usually the 2nd but can be others or more. The joint will have more pressure on it for a variety of reasons but most commonly from an elongated metatarsal with or without a hammer toe. In many cases a bunion can be present which may or may not be painful but often needs to be addressed as well. This condition must be differentiated from a nerve entrapment or both can be present.
Conservative Treatment – this is focused on reducing the inflammation and pain with ice, Rx topical cream, laser and sometimes injections. Strappings can also provide temporary relief and can be done in the office at time of visit. Orthotics also can be effective at removing the load to the affected joint. Sometimes oral steroids can be given for 5 days or so. Shockwave treatment is also another option. In rare cases, a walker boot can be given. Avoid any high heels at all. You must apply ice 4x/day for 15 minutes at a time or it will not help. NO exercise till your pain is gone by at least 90%. Can swim anytime though.
Surgical Options – this will depend on what deformities are present on the foot when reviewing x-rays. The goal is to remove the forces on the joint. Commonly a shortening osteotomy of the affected bone(s) is carried out and fixated with a screw. In some cases, if a bunion is present, this will have to be addressed as well because the first ray must be functional to take the load from walking or running. If a hammertoe is present this must also be addressed and this can be done via minimal incision technique (MIS) or standard technique. Also very often one of the main contributors of this problem is a tight heel cord or Achilles. If significant enough this will need to be lengthened by endoscopic technique. Post Op recovery is typically 48 hours of elevation, ice, and no weight bearing. Then into a cam boot for 4 weeks followed by graduated weight bearing in a stiff shoe or sneaker. Full activity in 3 months.
Peripheral Neuropathy
Neuropathy is a term used to describe any problem related to the nerves. Most problems in the legs are considered peripheral nerve problems meaning the CNS is not involved but in the legs themselves. Sometimes the lower back can contribute to the pain or neurologic symptoms in the leg and acts as a “double” crush. Think of nerves as a garden hose and the spigot is the spine and at the end of the hose are the toes. Any kink or “crush” of that hose/nerve will cause some damage and there can be multiple crushes, which can make things more difficult to achieve a successful treatment outcome. Diabetics are more prone to neuropathy and should be monitored regularly because if there is loss of sensation this can lead to ulcer, infection and even loss of limb. Many cases of neuropathy are often called idiopathic. This term means that there is no known cause. In most cases, this is NOT the case. Usually, there is an entrapment or compression of the nerve(s). A nerve entrapment can be easily identified by a peripheral nerve surgeon, when present in the leg. Dr. Ricciardi has been specially trained to diagnose and treat these problems. Many times other doctors will not be able to diagnose these nerve entrapments and often, special studies such as MRI or nerve conduction studies will not identify the problems. Also, if there is a history of carpal tunnel or arm nerve problems then it is more likely to be present in the legs.
Common sites of nerve entrapments in the legs:
- Tarsal Tunnel – this is like carpal tunnel in the wrist. The nerves on the inside of the ankle become stretch and compressed. This can be aggravated by flat, or hyper-pronated feet. The medial calcaneal nerve is also present here and can be a problem.
- Common Fibular Nerve – this is a nerve behind the head of the fibula near the knee. It is prone to entrapment and can also cause lower back pain and restless leg syndrome symptoms. Cramping in legs can also be present.
- Superficial Fibular Nerve – this is a branch of the common fibular nerve that is in the anterior-lateral leg and extends over the ankle into the foot. It is often injured in sports or ankle fractures but can also be a problem in athletes.
- Tibial Nerve – this nerve starts in the back of the knee and continues behind the calf muscles and eventually turns into the tarsal tunnel. Cramping is often present in the calf area.
- Deep Peroneal Nerve – this nerve is present on the top of the foot just below the ankle and can often be a problem with shoes or if there is a spur present near it.
- Saphenous and Sural Nerves – these are purely sensory and run on the inside and outside or the leg respectively. They can be injured during any surgery or injury.
Treatment if neuropathy/entrapments:
First, the proper diagnosis of the problem is made by a combination of the history, exam, and diagnostic testing. Many times there can be hormonal imbalances or other medical issues. Blood tests will often be ordered, and also a 3mm biopsy of the skin on the leg is often needed to rule out small fiber neuropathy, which is another kind of neuropathy. Diagnostic local anesthetic blocks are used to help isolate the involved nerves. In 70% of entrapment cases, surgical decompression is the treatment of choice in the other 30% they can respond to specialized physical therapy known as nerve gliding or nerve flossing. Topical prescription creams are also used to help with pain. In some cases, prescription vitamins are also prescribed as well as other medication to help deal with the pain of neuropathy. Most of the nerve surgeries are fairly quick surgeries and the patient is back to regular activity in a few weeks.
Toenail Fungus
Toenail fungus infections can be extremely unsettling and embarrassing, but they’re a lot more common than you might think. In fact, the American Academy of Dermatology estimates that about 12% of Americans are affected, with older adults especially likely to carry the pathogen.
Traditional treatments for fungal nails are spotty at best, and carry a risk of potentially serious side effects. However, cold laser therapy has dramatically improved the situation, and treatment is now much safer and boasts much higher success rates.
Do I Have Fungal Nails?
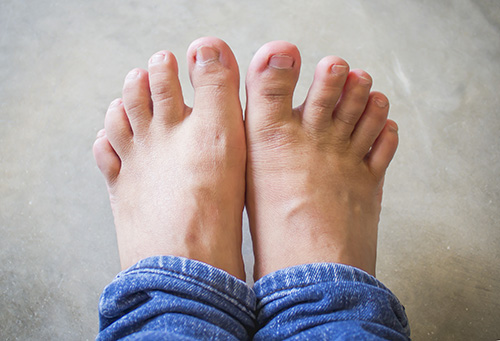
At the earliest stages of a fungal nail infection, you might notice a single whitish or yellowish mark under the tip of your toenail, or small ridges forming on the nail plate. As the condition worsens, symptoms include:
- Discoloration (typically anywhere from off-white and gray to yellowish or brownish)
- Thickening of the nail
- Ends of the nail becoming crumbly, ragged, or flakey
- Severe warping or distortion of the nail shape
- Odor
What Causes Fungal Nails?
Toenail fungus is caused by dermatophyte fungi—the same microorganisms responsible for athlete’s foot, ringworm, jock itch, and other common skin conditions. If you have athlete’s foot, the fungi can sometimes get underneath the nail through tiny cracks or cuts. It’s also possible to spread the fungi from person to person through indirect contact with infected surfaces—gym or pool floors, towels, even salon tools.
Zap Your Fungus with Laser Therapy
At Foot and Ankle Specialists of Nevada, advanced cold laser therapy is the treatment of choice for fungal nails, although we still offer older methods like oral and topical antifungal medications. It offers many advantages over previous procedures.
How It Works
The beams of light generated by the laser are tuned at a precise wavelength, power, and frequency that allows them to pass through the nail plate and attack the fungus underneath—all without harming your own cells. This makes it both highly safe and highly effective as a method of treatment.
One laser session requires about 30-45 minutes, though times can vary depending on how many toes are being treated and how severe the condition is. No anesthetic is required and you should not feel any pain or discomfort. Once the session is over, you can go right back home or to work—no down time. Some patients may only need a single treatment; however, as many as four treatments might be necessary to fully eradicate the fungus.
Once the fungus has been eliminated, a new, healthy, clear nail will grow out it its place. Although you will likely see some level of aesthetic improvement very quickly, it may take several months for the portion of the nail that has already been damaged to grow out and away.
Advantages Over Traditional Treatments
Compared to antifungal medications, laser treatment is:
- More effective. Cure rates for oral antifungals hover around 50-70 percent, and may be less effective in older patients or those with low circulation. Topicals are even less effective, since the medicine can’t really penetrate the nail plate. Laser treatment has provided much better results.
- Safer. Oral medications in particular carry a risk of side effects, including liver damage and failure. Some people tolerate them well; others do not. There are no known side effects or health risks with laser therapy.
- More convenient. A typical oral antifungal treatment regime requires 6-12 weeks of daily pills. Topicals may require up to a year of daily application, alongside thinning of the nail on a weekly basis. Laser requires just 1-4 sessions of 30-45 minutes.
Sports Injuries

Every physical activity carries with it a certain degree of risk. Because they’re not only responsible for supporting your entire weight but also powerfully propelling running strides, jumps, and cuts, feet and ankles are especially endangered.
Whenever your experience an injury in your lower extremity, make a point to see the team at the Foot & Ankle Specialists of Nevada. These incidents take away your ability to play, work, and move the way you want to, and ignoring them almost always makes the problem worse in the long run.
Injuring Your Feet and Ankles
Broadly speaking, there are two main types of foot and ankle injuries: traumatic (or acute) injuries, and overuse injuries.
Acute injuries happen in an instant—a big hit, a sudden stumble, an unfortunate hyperextension—and result in immediate (and often severe) pain and damage. On the other side, overuse injuries slowly build up over time, and dozens or hundreds of tiny impacts, stresses, and wear and tear weaken muscles, soft tissues, and bones.
Common causes of foot and ankle injuries include wearing improper shoes or equipment, rapidly changing your workout routine or increasing mileage/difficult too quickly, and not taking enough rest time between workouts.
Sports Injury Treatments that Work
Regardless of the type, location, or severity of your foot or ankle injury, our doctors are exceptionally qualified to diagnose and treat it. With a wide range of treatment options, spanning traditional conservative remedies to advanced technologies and state-of-the-art surgical techniques, our team will help you get back on your feet fast.
Tried-and-true treatments like rest, icing, compression wraps, elevation, stretching, and others still have their place in sports injury recovery, and are often part of a comprehensive treatment plan. In fact, they may even be sufficient on their own for minor injuries.
For tougher pain or more serious damage, we can provide a range of more aggressive (but still conservative!) treatments, including custom orthotics and technologies like laser and shockwave therapy. These cutting-edge options are often a great alternative to surgery, which is reserved only for the most serious cases.

When you hurt yourself on the sports field (or just going through life), you want a team in your corner. Because of our training and our expansive range of treatment options, we’re able to provide personalized and effective care. To schedule your appointment, give us a call at (702) 213-9093.
Nerve Pain
In a world of 24/7 communication, the sudden realization that your phone is dead can cause a sort of mini-panic. You might miss an important text!
Within your body, your peripheral nerves are the communications network, reporting sensory information back to the brain and issuing instructions to muscles and other organs. When nerves are damaged or impaired, pain is usually one of the primary indicators, but a wide variety of side effects and symptoms are possible. That includes strange sensations (tingling, burning, freezing, etc.), muscle weakness, or even complete numbness.
Because of their size, surroundings, and position, nerves in the lower legs, ankles, and feet tend to be the body’s most vulnerable.

Types of Lower Extremity Nerve Pain
The two of the most common categories of nerve pain we see at our office include:
- Peripheral neuropathy. This refers to a range of related conditions involving systemic damage or degeneration in peripheral nerves – usually in the feet. Like any other of the body’s systems, nerves need plenty of oxygen and nutrients to stay healthy. Low blood flow and high levels of sugar in the blood starve and poison nerves, which is why peripheral neuropathy is a very common complication of diabetes. Other potential causes include alcoholism, various diseases, and dietary deficits.
- Nerve compression. In order to reach all the way from the brain and spinal column to the furthest reaches of your feet and toes, nerves must navigate around muscles and bones, and even through narrow tunnels within joints. As a result, they are vulnerable to direct pressure from external or internal sources. Repetitive motions, tight clothing, weight gain, inflammation, injuries, bone misalignments, and host of other factors can all pinch, trap, or compress a nerve.
Treatments for Nerve Pain
Unlike your phone, getting the network back online after an issue isn’t always as easy as plugging in an adapter. Nerve damage from neuropathy or compression tends to worsen with time, and the longer you wait for treatment, the more likely the damage will be permanent, at least on some level.
For mild or early-stage cases, the first step will likely be conservative. Depending on the cause of your nerve pain, conservative care may take the form of medications (both oral pills and topical creams) physical therapy, custom orthotics, or even a change in footwear.
However, in the last several years a variety of new technologies and techniques have emerged to help manage (and even cure) nerve pain better than ever before. We are proud to offer these options to our patients.
- Electrical stimulation. This extremely promising and effective treatment option uses electrodes placed on the skin to generate a gentle electric current processed by your nerves. These electric signals provide numerous benefits, including inflammation reduction, improved blood flow, and increased cellular regeneration. In some cases, as the nerve fibers get used to receiving and transmitting these signals, they can actually begin to re-establish broken connections with other nerves and improve function.
- Nerve decompression surgery. In about 70% of cases where a nerve has been trapped, decompression surgery is the treatment of choice. Once we identify the precise source of the problem (using diagnostic techniques such as blood tests, biopsies, and local anesthetic blocks), we can perform the surgery. Most are fairly quick, and you can go back to your regular activities within just a few weeks.
- Laser therapy. Our cold laser can help soothe nerve pain and boost function by reducing inflammation and improving blood flow.
- Shockwave therapy. The high-pressure waves emanated by this tool have been shown to reduce the pain felt by nerve fibers.
No one is better equipped to identify and treat nerve pain conditions in the feet and ankles than the team at the Foot & Ankle Specialists of Nevada. To schedule your appointment with us at either of our area offices, please call (702) 878-2455.
