Peripheral Neuropathy
Neuropathy is a term used to describe any problem related to the nerves. Most problems in the legs are considered peripheral nerve problems meaning the CNS is not involved but in the legs themselves. Sometimes the lower back can contribute to the pain or neurologic symptoms in the leg and acts as a “double” crush. Think of nerves as a garden hose and the spigot is the spine and at the end of the hose are the toes. Any kink or “crush” of that hose/nerve will cause some damage and there can be multiple crushes, which can make things more difficult to achieve a successful treatment outcome. Diabetics are more prone to neuropathy and should be monitored regularly because if there is loss of sensation this can lead to ulcer, infection and even loss of limb. Many cases of neuropathy are often called idiopathic. This term means that there is no known cause. In most cases, this is NOT the case. Usually, there is an entrapment or compression of the nerve(s). A nerve entrapment can be easily identified by a peripheral nerve surgeon, when present in the leg. Dr. Ricciardi has been specially trained to diagnose and treat these problems. Many times other doctors will not be able to diagnose these nerve entrapments and often, special studies such as MRI or nerve conduction studies will not identify the problems. Also, if there is a history of carpal tunnel or arm nerve problems then it is more likely to be present in the legs.
Common sites of nerve entrapments in the legs:
- Tarsal Tunnel – this is like carpal tunnel in the wrist. The nerves on the inside of the ankle become stretch and compressed. This can be aggravated by flat, or hyper-pronated feet. The medial calcaneal nerve is also present here and can be a problem.
- Common Fibular Nerve – this is a nerve behind the head of the fibula near the knee. It is prone to entrapment and can also cause lower back pain and restless leg syndrome symptoms. Cramping in legs can also be present.
- Superficial Fibular Nerve – this is a branch of the common fibular nerve that is in the anterior-lateral leg and extends over the ankle into the foot. It is often injured in sports or ankle fractures but can also be a problem in athletes.
- Tibial Nerve – this nerve starts in the back of the knee and continues behind the calf muscles and eventually turns into the tarsal tunnel. Cramping is often present in the calf area.
- Deep Peroneal Nerve – this nerve is present on the top of the foot just below the ankle and can often be a problem with shoes or if there is a spur present near it.
- Saphenous and Sural Nerves – these are purely sensory and run on the inside and outside or the leg respectively. They can be injured during any surgery or injury.
Treatment if neuropathy/entrapments:
First, the proper diagnosis of the problem is made by a combination of the history, exam, and diagnostic testing. Many times there can be hormonal imbalances or other medical issues. Blood tests will often be ordered, and also a 3mm biopsy of the skin on the leg is often needed to rule out small fiber neuropathy, which is another kind of neuropathy. Diagnostic local anesthetic blocks are used to help isolate the involved nerves. In 70% of entrapment cases, surgical decompression is the treatment of choice in the other 30% they can respond to specialized physical therapy known as nerve gliding or nerve flossing. Topical prescription creams are also used to help with pain. In some cases, prescription vitamins are also prescribed as well as other medication to help deal with the pain of neuropathy. Most of the nerve surgeries are fairly quick surgeries and the patient is back to regular activity in a few weeks.
Wounds that Don’t Heal Need to be Checked
Your feet are covered a good part of the day. If you are diabetic, periodic screening is important for good health. Numbness is often another sign of diabetic foot and can mask a sore or wound.
Toenail Fungus
Toenail fungus infections can be extremely unsettling and embarrassing, but they’re a lot more common than you might think. In fact, the American Academy of Dermatology estimates that about 12% of Americans are affected, with older adults especially likely to carry the pathogen.
Traditional treatments for fungal nails are spotty at best, and carry a risk of potentially serious side effects. However, cold laser therapy has dramatically improved the situation, and treatment is now much safer and boasts much higher success rates.
Do I Have Fungal Nails?
At the earliest stages of a fungal nail infection, you might notice a single whitish or yellowish mark under the tip of your toenail, or small ridges forming on the nail plate. As the condition worsens, symptoms include:
- Discoloration (typically anywhere from off-white and gray to yellowish or brownish)
- Thickening of the nail
- Ends of the nail becoming crumbly, ragged, or flakey
- Severe warping or distortion of the nail shape
- Odor
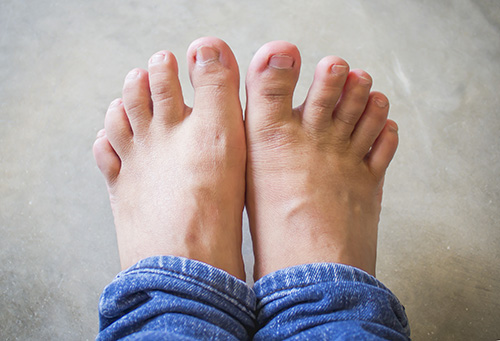
What Causes Fungal Nails?
Toenail fungus is caused by dermatophyte fungi—the same microorganisms responsible for athlete’s foot, ringworm, jock itch, and other common skin conditions. If you have athlete’s foot, the fungi can sometimes get underneath the nail through tiny cracks or cuts. It’s also possible to spread the fungi from person to person through indirect contact with infected surfaces—gym or pool floors, towels, even salon tools.
Zap Your Fungus with Laser Therapy
At Foot and Ankle Specialists of Nevada, advanced cold laser therapy is the treatment of choice for fungal nails, although we still offer older methods like oral and topical antifungal medications. It offers many advantages over previous procedures.
How It Works
The beams of light generated by the laser are tuned at a precise wavelength, power, and frequency that allows them to pass through the nail plate and attack the fungus underneath—all without harming your own cells. This makes it both highly safe and highly effective as a method of treatment.
One laser session requires about 30-45 minutes, though times can vary depending on how many toes are being treated and how severe the condition is. No anesthetic is required and you should not feel any pain or discomfort. Once the session is over, you can go right back home or to work—no down time. Some patients may only need a single treatment; however, as many as four treatments might be necessary to fully eradicate the fungus.
Once the fungus has been eliminated, a new, healthy, clear nail will grow out it its place. Although you will likely see some level of aesthetic improvement very quickly, it may take several months for the portion of the nail that has already been damaged to grow out and away.
Advantages Over Traditional Treatments
Compared to antifungal medications, laser treatment is:
- More effective. Cure rates for oral antifungals hover around 50-70 percent, and may be less effective in older patients or those with low circulation. Topicals are even less effective, since the medicine can’t really penetrate the nail plate. Laser treatment has provided much better results.
- Safer. Oral medications in particular carry a risk of side effects, including liver damage and failure. Some people tolerate them well; others do not. There are no known side effects or health risks with laser therapy.
- More convenient. A typical oral antifungal treatment regime requires 6-12 weeks of daily pills. Topicals may require up to a year of daily application, alongside thinning of the nail on a weekly basis. Laser requires just 1-4 sessions of 30-45 minutes.
Sports Injuries

Every physical activity carries with it a certain degree of risk. Because they’re not only responsible for supporting your entire weight but also powerfully propelling running strides, jumps, and cuts, feet and ankles are especially endangered.
Whenever your experience an injury in your lower extremity, make a point to see the team at the Foot & Ankle Specialists of Nevada. These incidents take away your ability to play, work, and move the way you want to, and ignoring them almost always makes the problem worse in the long run.
Injuring Your Feet and Ankles
Broadly speaking, there are two main types of foot and ankle injuries: traumatic (or acute) injuries, and overuse injuries.
Acute injuries happen in an instant—a big hit, a sudden stumble, an unfortunate hyperextension—and result in immediate (and often severe) pain and damage. On the other side, overuse injuries slowly build up over time, and dozens or hundreds of tiny impacts, stresses, and wear and tear weaken muscles, soft tissues, and bones.
Common causes of foot and ankle injuries include wearing improper shoes or equipment, rapidly changing your workout routine or increasing mileage/difficult too quickly, and not taking enough rest time between workouts.
Sports Injury Treatments that Work
Regardless of the type, location, or severity of your foot or ankle injury, our doctors are exceptionally qualified to diagnose and treat it. With a wide range of treatment options, spanning traditional conservative remedies to advanced technologies and state-of-the-art surgical techniques, our team will help you get back on your feet fast.
Tried-and-true treatments like rest, icing, compression wraps, elevation, stretching, and others still have their place in sports injury recovery, and are often part of a comprehensive treatment plan. In fact, they may even be sufficient on their own for minor injuries.
For tougher pain or more serious damage, we can provide a range of more aggressive (but still conservative!) treatments, including custom orthotics and technologies like laser and shockwave therapy. These cutting-edge options are often a great alternative to surgery, which is reserved only for the most serious cases.

When you hurt yourself on the sports field (or just going through life), you want a team in your corner. Because of our training and our expansive range of treatment options, we’re able to provide personalized and effective care. To schedule your appointment, give us a call at (702) 213-9093.
Nerve Pain
In a world of 24/7 communication, the sudden realization that your phone is dead can cause a sort of mini-panic. You might miss an important text!
Within your body, your peripheral nerves are the communications network, reporting sensory information back to the brain and issuing instructions to muscles and other organs. When nerves are damaged or impaired, pain is usually one of the primary indicators, but a wide variety of side effects and symptoms are possible. That includes strange sensations (tingling, burning, freezing, etc.), muscle weakness, or even complete numbness.
Because of their size, surroundings, and position, nerves in the lower legs, ankles, and feet tend to be the body’s most vulnerable.

Types of Lower Extremity Nerve Pain
The two of the most common categories of nerve pain we see at our office include:
- Peripheral neuropathy. This refers to a range of related conditions involving systemic damage or degeneration in peripheral nerves – usually in the feet. Like any other of the body’s systems, nerves need plenty of oxygen and nutrients to stay healthy. Low blood flow and high levels of sugar in the blood starve and poison nerves, which is why peripheral neuropathy is a very common complication of diabetes. Other potential causes include alcoholism, various diseases, and dietary deficits.
- Nerve compression. In order to reach all the way from the brain and spinal column to the furthest reaches of your feet and toes, nerves must navigate around muscles and bones, and even through narrow tunnels within joints. As a result, they are vulnerable to direct pressure from external or internal sources. Repetitive motions, tight clothing, weight gain, inflammation, injuries, bone misalignments, and host of other factors can all pinch, trap, or compress a nerve.
Treatments for Nerve Pain
Unlike your phone, getting the network back online after an issue isn’t always as easy as plugging in an adapter. Nerve damage from neuropathy or compression tends to worsen with time, and the longer you wait for treatment, the more likely the damage will be permanent, at least on some level.
For mild or early-stage cases, the first step will likely be conservative. Depending on the cause of your nerve pain, conservative care may take the form of medications (both oral pills and topical creams) physical therapy, custom orthotics, or even a change in footwear.
However, in the last several years a variety of new technologies and techniques have emerged to help manage (and even cure) nerve pain better than ever before. We are proud to offer these options to our patients.
- Electrical stimulation. This extremely promising and effective treatment option uses electrodes placed on the skin to generate a gentle electric current processed by your nerves. These electric signals provide numerous benefits, including inflammation reduction, improved blood flow, and increased cellular regeneration. In some cases, as the nerve fibers get used to receiving and transmitting these signals, they can actually begin to re-establish broken connections with other nerves and improve function.
- Nerve decompression surgery. In about 70% of cases where a nerve has been trapped, decompression surgery is the treatment of choice. Once we identify the precise source of the problem (using diagnostic techniques such as blood tests, biopsies, and local anesthetic blocks), we can perform the surgery. Most are fairly quick, and you can go back to your regular activities within just a few weeks.
- Laser therapy. Our cold laser can help soothe nerve pain and boost function by reducing inflammation and improving blood flow.
- Shockwave therapy. The high-pressure waves emanated by this tool have been shown to reduce the pain felt by nerve fibers.
No one is better equipped to identify and treat nerve pain conditions in the feet and ankles than the team at the Foot & Ankle Specialists of Nevada. To schedule your appointment with us at either of our area offices, please call (702) 878-2455.
Heel Pain
Every day, millions of Americans are greeting in the morning by intense heel pain. As a matter of fact, more than half of the population will suffer from significant heel pain at least once in their lives. We’re not talking about ordinary aches and pains here, but shooting, stabbing, even knife-like sensations that linger and persist for days and weeks.
Although heel pain is extremely common, it is not a normal part of life. Your feet are designed to provide a lifetime of locomotion, and when heel pain gets in the way of daily living, you need to see an expert who can help you heal.
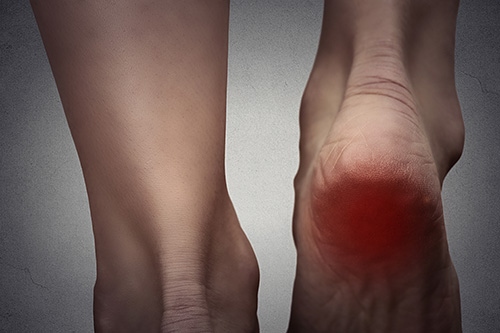
Causes of Heel Pain
Heel pain is not caused by a single condition, and usually can’t be traced to a single incident or injury. More likely, your heel pain is the result of multiple small traumas over time. Each step can place a force on heels equal to anywhere from one and a half to three times your own body weight. Days, weeks, even years of wear and tear from physically demanding occupations, athletic participation, and other activities will slowly build the pain and pressure.
Other Heel Pain Conditions
Some other conditions we treat frequently include:
Heel Pain Treatment Options
The good news is that, 9 out of 10 times, conservative treatments like icing, stretching, and custom orthotics will help you ease the pain of plantar fasciitis, along with most other forms of heel pain. For tougher pain, we may prescribe more aggressive treatments, including:
- Cortisone injections, which provide stronger pain relief to the aching tissues than over-the-counter medications.
- Shockwave therapy. This advanced technology uses high-intensity pressure waves to stimulate injured tissues, which reduces pain felt by nerve fibers, increases circulation, and triggers stem cells to accelerate the healing process.
- Cold laser therapy. The laser emits a beam of light tuned to a highly precise wavelength and intensity. At this frequency, the laser is able to penetrate deep into soft tissues to fight inflammation, improve blood flow, remove waste products, reduce pain, and stimulate tissue repair.
- For most heel pain conditions, surgery is a last resort that is only rarely required, for the most severe cases. The exception is tarsal tunnel syndrome, which is usually best treated with a decompression surgery.
It is critical to understand that not all heel pain is created equal. Even if the symptoms seem the same, the causes may be very different. Each case needs to be fully evaluated by an expert in order to ensure you get the most effective treatment.
Fractures
Breaking news: Foot and ankle fractures can lead to major pain, distress, and disruption in your life. Foot bones are tough, but they’re far from impervious to sudden impacts, severe twisting, auto accidents, or even just plain wear and tear.
If you break a bone in your foot or ankle, the last thing you want to do is keep walking on it. Get off your feet, get to the emergency room if you have to, and book an appointment with the Foot & Ankle Specialists of Nevada as soon as possible. We also take same day appointments.
Types of Fractures
Physicians classify fractures in many different ways—by location, bones effected, severity, etc. Generally speaking, there are three broad categories:
- Stress fractures are hairline cracks in the surface of a bone. They are usually caused by overuse and are common in load-bearing metatarsal bones of the arch. They usually don’t need surgery or even casting, but will need plenty of rest time to heal.
- Closed fractures. In closed fractures, the bone is “fully” broken, but has not broken the skin or done significant damage to the surrounding tissue. Closed fractures may be stable, in which the broken bone remains in the correct position and alignment, or unstable, in which at least one part of the bone has shifted out of place.
- Open fractures. Here, a significant unstable fracture has broken the skin and severely damaged surrounding soft tissue structures. If you experience an open fracture, you should attempt to stop the bleeding using firm pressure with a clean cloth, but you should not attempt to pop the bone back in place. Have someone call 911 immediately.
Signs That You May Have Broken a Bone
It’s not always immediately obvious that you’ve broken a bone. Often, stress fractures and stable closed fractures are shrugged off and misattributed to sprains. However, if you note any of the following symptoms, you should consider that a fracture is at least possible:
- Pain, often severe, at the site of the break
- Swelling
- Bruising
- Inability to walk or put weight on the foot
What to Do If You Suspect a Fracture
If you believe that a bone in your foot or ankle may be broken, it is important to avoid putting any weight on the foot and begin RICE treatment (Rest, Ice, Compression, and Elevation):
- Do not bear weight or aggravate the injury.
- Do this for about 20 minutes at a time, on and off, as necessary.
- An athletic wrap around the injury will help control swelling.
- Keep your feet propped up, over chest level if possible.
Next, you should contact our office and schedule an appointment as soon as possible. Fractures that are not treated properly can lead to post-traumatic arthritis, chronic pain and weakness, and other long-term complications and consequences.
Treating Foot and Ankle Fractures
Professional treatment from a physician will vary considerably based on the location and type of the break, as well as the extent of the damage to both bone and surrounding tissue. Your activity level, health, and long-term goals may also be a factor in determining the best treatment protocols.
- Stress fractures can usually be treated with simple rest. You can bear weight, but avoid running, playing sports, or engaging in any strenuous activities that would cause pain or aggravate the injury.
- Serious stress fractures and many closed, stable fractures may need an immobilization device—a leg cast, walking boot, or similar device. This will protect the bones from further damage while they heal.
- More complicated or at-risk fractures often require surgery to reposition and/or reconstruct the damaged bones. We may need to use hardware such as pins, screws, wires, or plates to hold the reconstructed bones and joints in place while they heal.
The board-certified physicians of the Foot & Ankle Specialists of Nevada have extensive training in both conservative and surgical treatment of foot and ankle fractures, including advanced techniques in reconstructive surgery. Although we always try to correct your issue non-invasively, we are equipped and trained to provide the best and most current treatment options, whatever your needs may be.
To schedule your appointment with our team in Las Vegas, NV, please call (702) 213-9093 today.
Child Foot Pain
In many ways, kids’ feet are very different from those of their parents. Softer bones, growing bodies, congenital deformities, and other factors mean they face very different challenges (and often require very different treatments) from adults.
There are advantages to this situation—kids generally recover quickly from injury, and some conditions may spontaneously improve without much treatment at all. However, since kids have their whole life ahead of them, it is extremely important that any foot conditions that could cause developmental issues or complications later in life are addressed immediately.
Do your child’s feet look strange or out of place? Are they experiencing any pain? Are they exhibiting strange walking gaits or behaviors? If so, make sure you bring them to the pediatric foot care experts at Foot & Ankle Specialists of Nevada.

Common Child Foot Pain Conditions
Although far from a comprehensive list, some of the most common pediatric conditions we treat include:
- Intoeing / Pigeon Toes. Your child walks with toes that appear pointed inward, and may also sit in the “reverse W” position. This condition may be caused by an inward rotation in the foot bones (metatarsus adductus), shin bones (tibial torsion), or hip bones (femoral anteversion). Some cases of intoeing may correct spontaneously without treatment, while others may require treatments such as physical therapy and orthotics.
- Flat Feet. Due to soft and flexible bones, children commonly have a flexible flat foot in which the arch “collapses” under body weight but returns in other circumstances. Most of the time, this corrects itself eventually. However, there are other congenital flat foot conditions (both flexible and rigid) that will not self-correct and will require treatments such as orthotics, stretching, physical therapy, or surgery.
- Toe Walking. An overly tight Achilles tendon or other developmental issue may cause your child to do most of their walking on tiptoes. If this continues to happen beyond age 2, your child should be evaluated. More serious treatment remedies (including physical therapy and potentially surgery) may be indicated if the problem persists until age 5 or 6.
- Heel Pain. Young adolescents, usually from about age 9 to 14, are especially susceptible to a heel pain condition known as Sever’s disease, or calcaneal apophysitis. At this age, the relatively soft growth plate of the heel bone is exposed and growing rapidly. This combined with a high level of physical activity may lead to swelling and irritation in the growth plate. Most of the time, this can be treated conservatively.
- Ingrown Toenails. In this condition, the corner or edge of a nail grows in rather than out, digging into soft flesh. This may produce pain or even an infection. Recurring ingrown toenails in kids is generally evidence of a genetic predisposition. We will remove the ingrown edge and then perform a chemical destruction of that part of the nail root. This keeps the problem from returning, and the procedure both has a high success rate and is usually not painful.
- Warts. Kids often develop warts on hands and feet, due to underdeveloped immune systems. Sometimes warts go away on their own, but if your child’s warts are causing pain, embarrassment, or have lasted for at least 6 months, they should be treated. We offer a range of options, including topical acid therapy, laser treatment, or sometimes oral medications. Deep, painful warts may need to be excised surgically.
Treating Your Children with Care and Compassion
Nothing is more important than the health of your child, and we strive to make our practice a welcoming and friendly atmosphere for both you and your child. From infants to teenagers, we offer advanced, evidence-based treatment solutions delivered with warmth and compassion.
To make an appointment with our team, complete an online contact form or give us a call at (702) 213-9093.

Bunions
What Is a Bunion?
Bunions are very common foot deformities that affect the side of the foot and the largest toe. A large, bony bump begins to form along the foot at the joint at the base of the great toe—where it meets the long midfoot bone known as the first metatarsal. At the same time, your large toe begins drifting in the opposite direction, pressing into (or even crossing over or under) the second toe.
Do You Need Surgery for Bunion Treatment?
Not everyone with a bunion necessarily requires a surgical procedure. The main goal of bunion treatment is to eliminate pain and allow you to function normally. In some cases, this can be accomplished with conservative treatments designed to reduce pressure on the bunion and improve alignment. Topical and oral medications, changes in your footwear, and orthotics are all potentially effective options.
That said, conservative treatments will not cure your bunion. If you find that you are still experiencing pain, discomfort, or mobility limitations, it is probably best to get your bunion fixed via surgery.

Bunion Surgery
There are many different types of bunion surgeries. The specific procedure or procedures used will be selected based on the severity of the condition itself, as well as any other considerations about your general health, personal goals, or activity level.
Silver Bunionectomy
This procedure may be selected for simple bunions with relatively minor alignment issues. We make a small incision at the bump, then remove the prominence using a special saw or burr.
The surrounding capsule is cut and tightened in order to help maintain the correction. Because the surgery is less invasive, recovery is much quicker—most people are back in regular shoes within a month.
Scarf Bunionectomy
This is the most common procedure we perform. In it, the surgeon cuts through the first metatarsal bone in the shape of a sideways Z. This allows the bone to be realigned and repositioned in a more natural state. Any remaining “bump” will be removed and the repaired joint held in place with two to three screws.
The initial recovery period for this procedure usually lasts about 48 hours. After that, you will be in a walking boot for up to four weeks before you can return to wearing normal shoes.
Full recovery generally takes about 3 months. During that time, we may recommend physical therapy, laser therapy, splints, topical creams, or pain medications if they are necessary.
Lapidus Fusion
A fusion may be selected in the case of more severe bunions, or those caused by hypermobility at the joint between the first metatarsal and medial cuneiform bones (the TMT joint) in the middle of the foot. Here, the affected joint is fused to provide stability.
During the procedure, cartilage lining the TMT joint is removed. Bones are then straightened, and held together using appropriate hardware (such as screws, plates, and/or staples). Part of the bunion bump may also be removed, and the capsule surrounding the joint is cut to help maintain the corrected alignment.
Lapidus fusion requires a somewhat longer recovery, with up to 4 weeks of total non-weight bearing after the procedure using a knee roller or cam walker boot. Return to regular shoes may require 3 to 4 months, depending on swelling.
Additional Surgical Procedures
Sometimes, the surgeon may need to perform a secondary procedure alongside the main bunion surgery in order to provide the best outcome. The decision may need to be made at the time of surgery. These might include:
- Akin Osteotomy—a small wedge of bone is removed from the big toe in order to allow it to lie straight. This may be done with a minimally invasive approach, or using traditional staple fixation.
- Sesamoid Removal—the two tiny sesamoid bones act as “pulleys” underneath the big toe joint to help generate power. However, they often become dislocated as a result of a bunion. One of both may need to be removed.
- Second Toe Surgery—sometimes, the surgeon will also need to correct a dislocated second toe or perform other surgical procedures as needed. The need for a second toe surgery may not be apparent until the actual surgery is in progress. Any such decisions are made with your best interests in mind.
Our doctors offer extensive experience, specialized training, and board certifications in complex foot reconstruction and fixation techniques. We are proud to report a 95% success rate with our bunion surgeries. Among those who get bunion surgery, fewer than 1 in 20 suffer a recurrence.
If you are struggling with bunion pain, contact us for a consultation and discussion of your treatment options. You can schedule at our offices by dialing 702) 213-9093.
Ankle Pain

Chronic ankle pain, especially on the lateral (outside) side of the joint, is a major source of distress for active individuals of all ages. Sufferers in their 20s and 30s may find that the pain forces them to cut back on sports and fitness activities. People of all ages may also feel unstable on their feet, with the ankles constantly feeling as if they will give way at any instant. Acute pain might spike with certain motions or activities; chronic pain may set in and stay for hours or days.
This kind of pain is a lot more common than you might think. By some estimates, as many as 40% of all ankle sprain suffers will deal with some amount of chronic ankle pain well after “full healing.” There could be other contributing factors as well.
Causes of Chronic Ankle Pain
Chronic ankle pain and instability usually results after an ankle sprain that never healed properly, or perhaps a series of sprains. When ligaments are stretched or torn, it takes time and effort during rehabilitation to rebuild strength. That process may, unfortunately, be left incomplete. With each injury, the ligaments come back a little bit looser and weaker, and aren’t as able to protect you from the next injury.
This is a big problem, as many people who suffer ankle sprains do not initially take their injury as seriously as they should. Don’t try to “walk it out” or assume the injury will heal on its own. Seeking professional advice is always a must.
That said, sprains and weak ligaments are not the only possible cause of chronic ankle pain. Other suspects include:
- Nerve injuries or compression
- Arthritis
- Bone fractures
- Inflammation in other soft tissues, such as tendons or joint lining
- Built-up scar tissue in the joint

Treatment and Restoration for Ankle Pain
Our team understands that each person and each condition are different. The best treatment plan for you personally may vary based on the cause and severity of your chronic ankle pain, as well as your personal and professional needs.
Treatment options may include:
- Physical therapy. Stretches and exercises are designed to relieve pain, increase range of motion, and improve strength and stability in the supporting muscles and tendons. This can provide temporary support to a weak or unstable ankle.
- Shockwave therapy. This advanced device uses high-intensity pressure waves to reduce pain and stimulate healing.
- Laser treatment. Our state-of-the-art cold laser improves oxygen transfer, tissue repair, and soothes pain.
- Nerve decompression. May be necessary if your chronic pain is caused by a nerve issue.
When you visit our practice, you can expect a thorough examination, accurate diagnosis, and individual treatment from the best trained specialists in the area. To schedule your appointment, please call (702) 878-2455.

